
It wasn’t by accident that travel nurse team, Jessica Frates and Istok Miralem, ended up working in America’s COVID-19 epicenter, New York City. They chose the NYC assignment out of a hunch they had already contracted the virus themselves, and they knew they could help by going there.
“We did some traveling in Amsterdam and Spain,” Jessica explains. “After that trip, we got really sick for about two weeks. We didn’t get tested, but the symptoms were pretty dead on.”
“I don’t know how much scientific evidence there is behind it,” adds Istok, “that if you have had COVID, you can’t get it again. But we felt like, ‘We got really sick that time, maybe we can’t get it again, so let’s just go right into the fire.’”
And even if what they had wasn’t coronavirus, they reasoned that being in healthcare, they would likely be exposed eventually anyway. “Why not go to a place that we can start working and be exposed, so we can continue working in all the other states and help out anywhere we can,” Jessica says.
Travel nursing with a co-pilot

Both Istok and Jessica are veteran nurses, he with nine years’ experience, she close to eight. The New York assignment was her first travel job. Istok had been a travel nurse for nearly five years. It was on a Rhode Island assignment that Istok met Jessica.
“I was a floater at Rhode Island Hospital,” Istok explains. “I went to various floors and saw her and couldn’t leave without her.”
They started hanging out, then dating, and it wasn’t long before he convinced her to try travel nursing.
“Istok kind of stole me,” Jessica says. “I had the idea of wanting to try travel nursing in the past, but I was kind of scared and didn’t want to do it on my own. Then we started dating, and I said, ‘OK, I’ll try it with you.’ At least, I have a copilot now!”
She adds, “We’ve had it really lucky. We’ve been able to get on the same schedule, driving into work together, working on the same unit together. I don’t know if we will ever be so blessed again to have it this good, but we are really enjoying it.”
RELATED: Travel nurses strengthen their indelible bond fighting COVID-19
Caring for patients under COVID-19 protocols
Jessica’s background is med surg nursing. Istok started off in a progressive care unit focused predominantly on telemetry and cardiac surgery. In New York City, they’re serving in a designated COVID unit, so all their patients are COVID patients. It has been a major change from treating the pneumonia, flu, renal failure, and heart failure patients they typically care for. Life under pandemic protocols definitely has upended their normal routine.
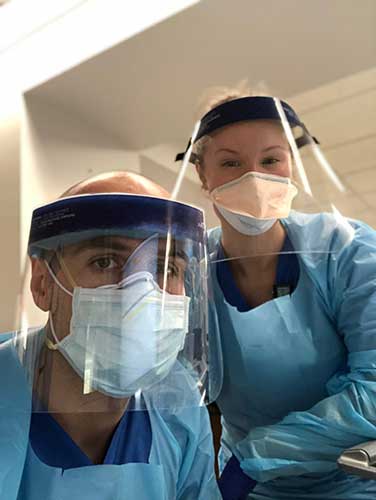
“As far as the unit we are on, we’re not in the thick of it, the crazy part,” says Jessica. “Our roommates are ICU nurses, and they are seeing some really crazy stuff. We are seeing a lot of people that are on high oxygen requirements, but we haven’t had any deaths, thankfully.”
One challenge they faced came from the standard protocol of changing personal protective equipment for each patient, which wasted a lot of time and used a lot of supplies. Like the rest of the staff, they soon learned to conserve while being more efficient. Always garbed in PPE on the floor, they ceased changing out gowns and shields, but did change out gloves or they’d double-glove.
The shortage of ventilators also meant changing the way they treat their patients. “Alongside the rest of healthcare, we are learning how to treat patients that are COVID positive and where their threshold is for oxygenation or intubation,” Istok says. “We are acting completely differently than we normally would for patients on oxygen. We really manage those with low SAT (oxygen saturation) levels and try to keep them so they don’t get vented.”
Jessica elaborates, “We’re managing patients with oxygen saturations in the low 80s, high 70s, and that is not something we typically do.”
Emotional support for patients in isolation
They’ve also responded like never before to a need from patients for emotional support while in isolation.
“Being there for patients when their family cannot — we really become their family,” Istok explains. “When you can’t see your loved ones for isolation reasons, healthcare workers are really vital in a role of guidance and just being there. Even though we’re distanced with all the layers of PPE making it hard to show warmth, I’ve tried to be warmer and be more present.”
Jessica and Istok are themselves at the receiving end of great emotional support from the people they work with, so touched by how enthusiastically the hospital staff has taken to them. “Everyone is grateful to have us. It’s charming how welcoming all the staff is.”
Everything closed except NYC’s heart

One disappointment has to do with the very thing many travel nurses live for — using their off-time to explore the area. Most everything in the Big Apple is closed — from tourist attractions like the Statue of Liberty to the Museum of Modern Art to all the fascinating shops, theatres, food carts, delis, bodegas, and world-famous restaurants that make NYC so exciting.
“They say this is the city that never sleeps,” Jessica jokes. “Well, it’s finally sleeping.”
Of course, what they do experience, they can enjoy without crowds, like strolling Central Park or the Brooklyn Bridge. Plus they’re happy to do without the city’s noisy, frantic, nerve-jangling traffic congestion: “There is no traffic, and when you get every green light down the main road, we call it, ‘riding the green lights all the way down’.”
They’ve experienced another rare thrill, one whose memory will put a lump in their throats for the rest of their lives with love for a great city.
“Seven p.m. every night, everyone is honking their horns, clapping, and cheering for all the healthcare and essential workers in the city,” Jessica says. “It’s awesome. You can hear it all the way from Central Park where I was walking yesterday.”
“Of course,” she adds, “we join in too.”
Interested in learning more about travel nursing? Call us for more information at 800.866.0407 or view today’s job openings.










